Journal of Jilin University(Medicine Edition) ›› 2026, Vol. 52 ›› Issue (1): 171-181.doi: 10.13481/j.1671-587X.20260118
• Research in basic medicine • Previous Articles Next Articles
Effect of USF2 knockdown on coagulation dysfunction in septic rats and its mechanism
Jingyuan WANG,Fang CHEN,Yancun LIU,Shixin LI,Songtao SHOU( )
)
- Department of Emergency Medicine General Hospital,Tianjin Medical University,Tianjin 300052,China
-
Received:2025-02-17Accepted:2025-03-26Online:2026-01-28Published:2026-02-24 -
Contact:Songtao SHOU E-mail:zyyshou@tmu.edu.cn
CLC Number:
- R631.2
Cite this article
Jingyuan WANG,Fang CHEN,Yancun LIU,Shixin LI,Songtao SHOU. Effect of USF2 knockdown on coagulation dysfunction in septic rats and its mechanism[J].Journal of Jilin University(Medicine Edition), 2026, 52(1): 171-181.
share this article
Tab.2
Expression levels of USF2 mRNA and protein in lung and appendix tissues of rats in various groups"
| Group | Lung tissue | Appendix tissue | ||
|---|---|---|---|---|
| USF2 mRNA | USF2 protein | USF2 mRNA | USF2 protein | |
| Control | 0.26±0.02 | 0.33±0.01 | 0.32±0.01 | 0.25±0.03 |
| Model | 1.64±0.01* | 1.49±0.03* | 1.52±0.03* | 1.77±0.01* |
| Positive drug | 1.61±0.03* | 1.48±0.02* | 1.48±0.01* | 1.78±0.01* |
| Si-NC | 1.60±0.01* | 1.47±0.01* | 1.49±0.02* | 1.80±0.02* |
| Si-USF2 | 0.53±0.01*△# | 0.60±0.03*△# | 0.66±0.02*△# | 0.58±0.01*△# |
| JNK activator | 0.56±0.02*△# | 0.58±0.02*△# | 0.65±0.01*△# | 0.59±0.01*△# |
Tab.3
PLT counts and coagulation function parameters of rats in various groups"
| Group | PLT(×109 L-1) | APTT(t/s) | PT(t/s) | TT(t/s) | DD [ρB/(mg·L-1)] | FIB [ρB/(g·L-1)] |
|---|---|---|---|---|---|---|
| Control | 732.56±0.02 | 21.25±0.01 | 11.25±0.01 | 14.25±0.01 | 0.21±0.01 | 5.98±0.02 |
| Model | 354.17±0.01* | 35.68±0.02* | 28.47±0.02* | 25.69±0.02* | 1.81±0.02* | 1.25±0.06* |
| Positive drug | 401.25±0.01*△ | 31.58±0.01*△ | 25.47±0.02*△ | 21.14±0.02*△ | 1.54±0.02*△ | 1.69±0.05*△ |
| Si-NC | 353.25±0.02* | 35.58±0.02* | 28.45±0.01* | 25.47±0.02* | 1.81±0.02* | 1.24±0.06* |
| Si-USF2 | 698.25±0.09*△# | 24.14±0.03*△# | 15.24±0.01*△# | 17.84±0.02*△# | 0.67±0.03*△# | 4.74±0.02*△# |
| JNK activator | 547.36±0.08*△#○ | 28.26±0.02*△#○ | 20.14±0.02*△#○ | 20.14±0.01*△#○ | 1.12±0.02*△#○ | 2.58±0.03*△#○ |
Tab.4
Levels of IL-1β, IL-6, TNF-α, CRP, and PCT in serum of rats in various groups [n=10, x±s, ρB/(ng·L-1)]"
| Group | IL-1β | IL-6 | TNF-α | CRP | PCT |
|---|---|---|---|---|---|
| Control | 26.51±0.42 | 32.17±0.75 | 38.01±0.37 | 24.58±0.49 | 20.67±2.52 |
| Model | 93.42±1.64* | 83.71±1.41* | 95.14±1.55* | 81.45±1.07* | 37.12±5.81* |
| Positive drug | 85.07±1.52*△ | 76.82±1.03*△ | 83.04±1.13*△ | 67.51±1.12*△ | 26.35±3.63△ |
| Si-NC | 94.73±1.58* | 84.97±1.25* | 94.62±1.23* | 81.78±1.04* | 36.18±6.07* |
| Si-USF2 | 51.58±0.96*△# | 44.76±0.89*△# | 45.28±0.69*△# | 37.34±1.01*△# | 23.40±3.90△# |
| JNK activator | 70.25±1.01*△#○ | 62.90±2.34*△#○ | 65.35±1.85*△#○ | 52.36±1.27*△#○ | 30.06±5.77*△#○ |
Tab.5
SOD activities and GSH and MDA levels in serum of rats in various groups"
| Group | SOD [λB/(U·mL-1)] | GSH [cB/(μmol·L-1)] | MDA [cB/(nmol·L-1)] |
|---|---|---|---|
| Control | 158.35±0.25 | 74.58±0.47 | 15.69±0.24 |
| Modle | 25.69±0.35* | 14.25±0.14* | 58.69±0.21* |
| Positive drug | 30.24±0.49*△ | 21.47±0.23*△ | 47.58±0.31*△ |
| Si-NC | 25.68±0.34* | 14.23±0.12* | 58.68±0.19* |
| Si-USF2 | 98.74±0.65*△# | 57.48±0.36*△# | 29.87±0.25*△# |
| JNK activator | 85.47±0.61*△#○ | 41.25±0.74*△#○ | 41.25±0.34*△#○ |
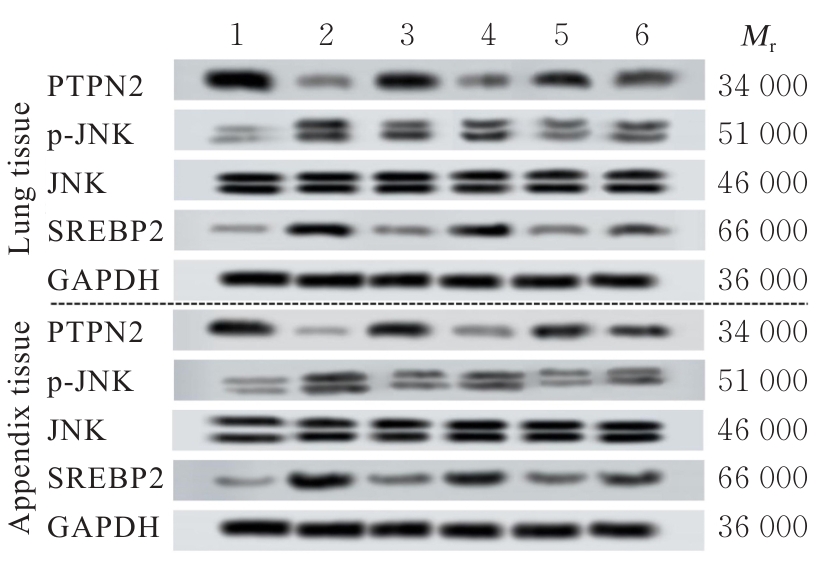
Tab.6
Expression levels of PTPN2, p-JNK, JNK, and SREBP2 proteins in lung and appendix tissues of rats in various groups"
| Group | Lung tissue | Appendix tissue | ||||
|---|---|---|---|---|---|---|
| PTPN2 | p-JNK/JNK | SREBP2 | PTPN2 | p-JNK/JNK | SREBP2 | |
| Control | 3.65±0.05 | 0.54±0.12 | 0.51±0.04 | 3.46±0.12 | 0.15±0.08 | 0.24±0.06 |
| Model | 1.21±0.09* | 2.53±0.03* | 3.02±0.05* | 1.27±0.05* | 1.36±0.06* | 1.30±0.05* |
| Positive drug | 1.75±0.11*△ | 2.19±0.06*△ | 2.28±0.05*△ | 1.80±0.07*△ | 0.98±0.07*△ | 1.01±0.03*△ |
| Si-NC | 1.27±0.06* | 2.50±0.06* | 3.06±0.04* | 1.35±0.08* | 1.35±0.06* | 1.28±0.08* |
| Si-USF2 | 2.62±0.04*△# | 1.16±0.08*△# | 1.67±0.07*△# | 3.01±0.06*△# | 0.58±0.04*△# | 0.62±0.06*△# |
| JNK activator | 1.91±0.13*△#○ | 1.75±0.10*△#○ | 2.09±0.11*△#○ | 2.06±0.05*△#○ | 0.88±0.03*△#○ | 0.95±0.07*△#○ |
| [1] | LAZAR A. Recent data about the use of corticosteroids in sepsis-review of recent literature[J]. Biomedicines, 2024, 12(5): 984. |
| [2] | REN C, LI Y X, XIA D M, et al. Sepsis-associated coagulopathy predicts hospital mortality in critically Ill patients with postoperative sepsis[J]. Front Med (Lausanne), 2022, 9: 783234. |
| [3] | GAO S, ZHANG Z, WANG X, et al. hsa-miR-875-5p inhibits tumorigenesis and suppresses TGF-β signalling by targeting USF2 in gastric cancer[J]. J Transl Med, 2022, 20(1): 115. |
| [4] | DONG W, LIAO R, WENG J, et al. USF2 activates RhoB/ROCK pathway by transcriptional inhibition of miR-206 to promote pyroptosis in septic cardiomyocytes[J]. Mol Cell Biochem, 2024, 479(5): 1093-1108. |
| [5] | HONGDUSIT A, FOX J M. Optogenetic analysis of allosteric control in protein tyrosine phosphatases[J]. Biochemistry, 2021, 60(4): 254-258. |
| [6] | MENG H, ZHAO H, CAO X, et al. Double-negative T cells remarkably promote neuroinflammation after ischemic stroke[J]. Proc Natl Acad Sci U S A, 2019, 116(12): 5558-5563. |
| [7] | ALKAFAAS S S, KHEDR S A, ELKAFAS S S, et al. Targeting JNK kinase inhibitors via molecular docking: A promising strategy to address tumorigenesis and drug resistance[J]. Bioorg Chem, 2024, 153: 107776. |
| [8] | GUO C, CHI Z, JIANG D, et al. Cholesterol Homeostatic Regulator SCAP-SREBP2 Integrates NLRP3 Inflammasome Activation and Cholesterol Biosynthetic Signaling in Macrophages[J]. Immunity, 2018, 49(5): 842-856. |
| [9] | LI Y, ZHOU H, LI Y, et al. PTPN2 improved renal injury and fibrosis by suppressing STAT-induced inflammation in early diabetic nephropathy[J]. J Cell Mol Med, 2019, 23(6): 4179-4195. |
| [10] | GONG M, LIANG W, LU Q, et al. PHLDA1 knockdown inhibits inflammation and oxidative stress by regulating JNK/ERK pathway, and plays a protective role in sepsis-induced acute kidney injury[J]. Allergol Immunopathol (Madr), 2022, 50(6): 1-9. |
| [11] | 周艳君, 陈洁, 张静航, 等. 2011-2019年湖南省男男性行为人群哨点HIV、梅毒感染状况及性行为特征趋势分析[J]. 实用预防医学, 2023, 30(6): 641-646. |
| [12] | 吴丹. 辛伐他汀对脓毒症大鼠心肌保护作用的实验研究[D]. 南昌:南昌大学, 2011. |
| [13] | XIE Y, LI X, DENG W, et al. Knockdown of USF2 inhibits pyroptosis of podocytes and attenuates kidney injury in lupus nephritis[J]. J Mol Histol, 2023, 54(4): 313-327. |
| [14] | 张国明, 王禹, 李天德, 等. 应激活化蛋白激酶在大鼠缺血后适应中的变化及其对细胞凋亡影响的研究[J]. 浙江大学学报(医学版), 2009, 38(6): 611-619. |
| [15] | EVANS L, RHODES A, ALHAZZANI W, et al. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock 2021[J]. Intensive Care Med, 2021, 47(11): 1181-1247. |
| [16] | COHEN J, VINCENT J L, ADHIKARI N K, et al. Sepsis: a roadmap for future research[J]. Lancet Infect Dis, 2015, 15(5): 581-614. |
| [17] | LIU F, WANG X, ZHENG B, et al. USF2 enhances the osteogenic differentiation of PDLCs by promoting ATF4 transcriptional activities[J]. J Periodontal Res, 2020, 55(1): 68-76. |
| [18] | SUN J, GE X, WANG Y, et al. USF2 knockdown downregulates THBS1 to inhibit the TGF-β signaling pathway and reduce pyroptosis in sepsis-induced acute kidney injury[J]. Pharmacol Res, 2022, 176: 105962. |
| [19] | LYONS P G, MICEK S T, HAMPTON N, et al. Sepsis-associated coagulopathy severity predicts hospital mortality[J]. Crit Care Med, 2018, 46(5): 736-742. |
| [20] | VARDON-BOUNES F, RUIZ S, GRATACAP M P, et al. Platelets are critical key players in sepsis[J]. Int J Mol Sci, 2019, 20(14): 3494. |
| [21] | LEISMAN D E, DOERFLER M E, WARD M F, et al. Survival benefit and cost savings from compliance with a simplified 3-hour sepsis bundle in a series of prospective, multisite, observational cohorts[J]. Crit Care Med, 2017, 45(3): 395-406. |
| [22] | WAUTHIER L, FAVRESSE J, HARDY M, et al. D-dimer testing: a narrative review[J]. Adv Clin Chem, 2023, 114: 151-223. |
| [23] | MACKIE I, CASINI A, PIETERS M, et al. International council for standardisation in haematology recommendations on fibrinogen assays, thrombin clotting time and related tests in the investigation of bleeding disorders[J]. Int J Lab Hematol, 2024, 46(1): 20-32. |
| [24] | LI C T, WANG H B, XU B J. A comparative study on anticoagulant activities of three Chinese herbal medicines from the genus Panax and anticoagulant activities of ginsenosides Rg1 and Rg2[J]. Pharm Biol, 2013, 51(8): 1077-1080. |
| [25] | AHMAD I, SHARMA S, GUPTA N, et al. Antithrombotic potential of esculin 7, 3', 4', 5', 6'-O-pentasulfate (EPS) for its role in thrombus reduction using rat thrombosis model[J]. Int J Biol Macromol, 2018, 119: 360-368. |
| [26] | KAO S Y, TSAO C M, KE H Y, et al. Loss of plasma fibrinogen contributes to platelet hyporeactivity in rats with septic shock[J]. Thromb Res, 2024, 241: 109072. |
| [27] | TANG B, YAO J, WU S, et al. Efficacy of urinary trypsin inhibitor in the treatment of rats with severe sepsis and its effects on coagulation and immunity[J]. Mol Cell Toxicol, 2023, 19(4): 753-765. |
| [28] | MARTINS P S, BRUNIALTI M K, MARTOS L S, et al. Expression of cell surface receptors and oxidative metabolism modulation in the clinical continuum of sepsis[J]. Crit Care, 2008, 12(1): R25. |
| [29] | SALOMÃO R, FERREIRA B L, SALOMÃO M C, et al. Sepsis: evolving concepts and challenges[J]. Braz J Med Biol Res, 2019, 52(4): e8595. |
| [30] | WANG X, WU F P, HUANG Y R, et al. Matrine suppresses NLRP3 inflammasome activation via regulating PTPN2/JNK/SREBP2 pathway in sepsis[J]. Phytomedicine, 2023, 109: 154574. |
| [1] | Kun YANG,Qianyao FU,Yongqiang SUN,Kun YANG,Jun MENG. Protective effect of dexmedetomidine on intestinal mucosal injury in rats with enterogenous sepsis and its mechanism [J]. Journal of Jilin University(Medicine Edition), 2025, 51(4): 855-865. |
| [2] | Chongyang ZHANG,Jia LUO,Xue QIN,Panxi SUN,Lili WEI,Xiushi YU. Protective effect of prunetin on cerebral ischemia-reperfusion injury in rats by regulating JNK/p38 pathway [J]. Journal of Jilin University(Medicine Edition), 2025, 51(2): 296-306. |
| [3] | Donghui LIU,Mingxi ZHANG,Wenliang FU,Xiumei FU,Chengjun SONG,Zhihong CHEN. Effects of sericin on injury of podocytes induced by high glucose and JNK signaling pathway [J]. Journal of Jilin University(Medicine Edition), 2022, 48(6): 1403-1410. |
| [4] | YUE Yuan, XU Yinglian, WANG Jingjing, SUN Minying, ZHANG Zenan, ZHAO Xinyue, LI Zongpu, TAI Guixiang. Inhibitory effects of down-regulation of JNK enzymatic activity on growth of human prostate cancer cells, hepatocellular carcinoma cells and breast cancer cells [J]. Journal of Jilin University(Medicine Edition), 2019, 45(05): 1046-1051. |
| [5] | WANG Tu, SUN Xiaoxu, CHEN Long, CUI Haipeng, LIU Kai, XIE Yaqin, LI Ying, ZHAO Juan. Effect of Urantide on expression of c-Jun N-terminal kinase in thoracic aorta tissue of rats with atherosclerosis and its significance [J]. Journal of Jilin University(Medicine Edition), 2019, 45(04): 813-818. |
| [6] | ZHENG Guilang, GUO Yuxiong, LYU Juanjuan, HUANG Jinda, LIU Cui, ZENG Qiyi. Protective effect of overexpression of uncoupling protein 2 on mitochondria in cardiomyocytes of rats with sepsis [J]. Journal of Jilin University Medicine Edition, 2018, 44(04): 698-703. |
| [7] | QIU Lijie, ZHANG Ye, ZHANG Wenjing, QIAN Donghua. Meta-analysis on curative effects of statins in treatment of pneumoniaor or sepsis [J]. Journal of Jilin University Medicine Edition, 2016, 42(02): 336-344. |
| [8] | LU Feiping, CHEN Wei, ZHEN Jie, MA Li. Changes of lymphocyte subsets in elderly patients with sepsis before and after immune modulation therapy [J]. Journal of Jilin University Medicine Edition, 2015, 41(05): 994-997. |
| [9] | WANG Zihang, ZHANG Yuhong, XIA Daozi, LI Guangsen, WU Jun, YOU Yue, HUANG Dongmei, BO Huaying, HU Bin, MAO Xin. Inhibition of expression of JNK1 in mouse hepatocellular carcinoma cell lines and cell migration and invasion mediated by ultrasound-targeted microbubble destruction [J]. Journal of Jilin University Medicine Edition, 2015, 41(01): 21-26. |
| [10] | ZHANG Yu-Gong, Tang-Jian-Wu, Wang-Chao-Qing, Wang-Zhi-Jiang, SUN Cheng-Rong, WANG Mei, WANG Bei. Inhibitory effects of shRNA on expression of JNK |in mouse hepatocellular carcinoma cell lines and cell migration and invasion [J]. J4, 2009, 35(3): 410-414. |
|
||