| [1] |
Zhongwei ZHOU,Wei DU,Yu NING,Jing YU,Fengyou GUO,Xueliang YANG.
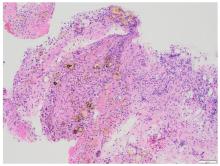
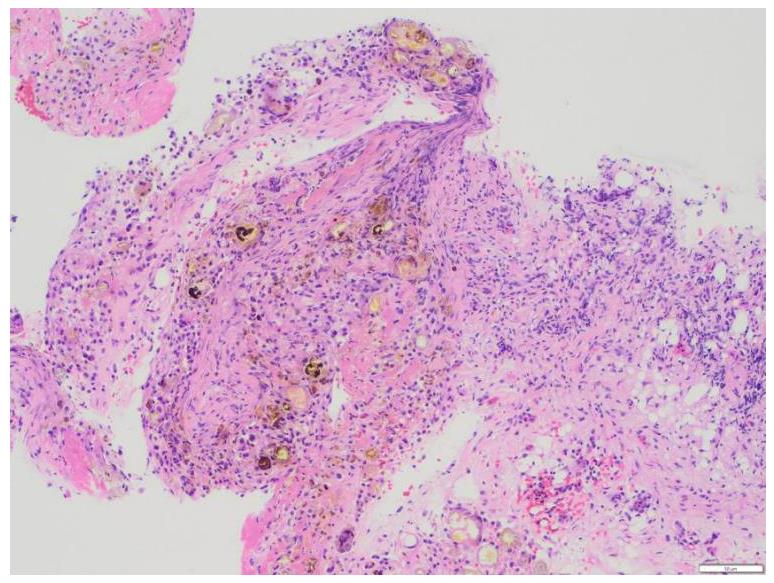
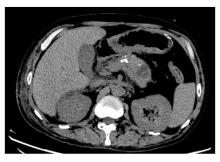
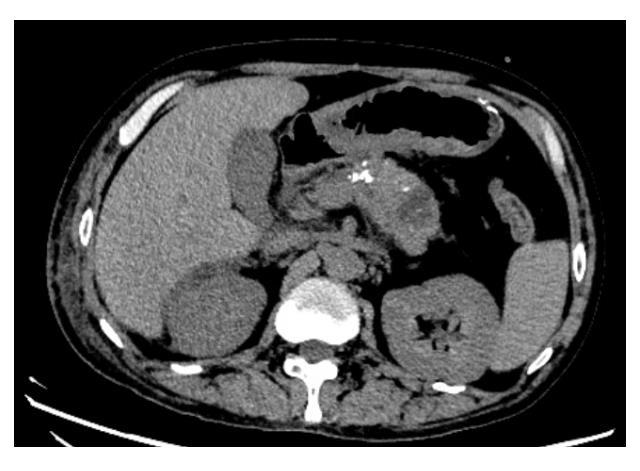
SMARCB1/INI1-deficient undifferentiated pancreatic carcinoma: A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2026, 52(2): 523-529.
|
| [2] |
Lei TIAN, Yuyan LIU, Yuqing WANG, Zhiyu ZHANG, Xiumei SUN.
Grade Ⅲ open bite complicated with tongue hypertrophy treated by mandibular incisor extraction:A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2026, 52(1): 236-245.
|
| [3] |
Shuangji LI,He SHI,Yiwen QIN,Xiang LI,Yuyang LI,Weiwei LIU,Jia LI.
Desmoplastic fibroma of mandible: A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2026, 52(1): 246-251.
|
| [4] |
Lei SUN,Yong YU,Xiaojun LIU,Sheng MIAO.
46, XX male sex reversal syndrome:A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2026, 52(1): 252-256.
|
| [5] |
Yi LIU,Qingguang MENG, Hugejile,Yang QU.
Spinal gout patient with intervertebral disc involvement and nerve compression treated with unilateral biportal endoscopic surgery: A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2026, 52(1): 257-263.
|
| [6] |
Qian AO,Jingting LI,Nan LIANG,Hui SUN.
Recurrent follicular variant of papillary thyroid carcinoma with DICER1 mutation in adolescent:A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2025, 51(6): 1702-1708.
|
| [7] |
Pengqing WU,Lingpeng ZENG,Zhaoxia LUO,Yangyang LEI,Ruiqin GOU,Qing ZHANG.
Thymus physiological uptake in patient with differentiated thyroid carcinoma after postoperative iodine-131 treatment: A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2025, 51(5): 1358-1362.
|
| [8] |
Geer A,Qin WANG,Lijing JIAO,Hailun ZHOU,Shanshan GAN,Yang HAN,Ruichao LIU,Yabin GONG.
Research progress in effects of CD4+T cell-mediated immune tolerance on occurrence and development of malignant pleural effusion
[J]. Journal of Jilin University(Medicine Edition), 2025, 51(4): 1121-1128.
|
| [9] |
Xiangjin HU,Xiumei SUN,Kai CHEN,Guomin WU.
Changes of upper airway in patient with skeletal class Ⅱ malocclusion accompanied by OSAHS after maxillomandibular advancement surgery: A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2025, 51(2): 493-500.
|
| [10] |
Qi ZHANG,Xiaoyuan XU,Yumiao WU,Han ZHANG,Zhiqiang HU,Jiamin YUAN,Yuchen CUI,Xianchun ZHU.
Treatment of skeletal class Ⅱ high angle malocclusion patient by clear aligner therapy combined with orthognathic surgery: A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2025, 51(2): 508-515.
|
| [11] |
Luyao WANG,Chenxi ZHAO,Wanze ZHANG,Linlin LIU.
Second primary tracheal adenoid cystic carcinoma:A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2025, 51(1): 215-221.
|
| [12] |
Jinping ZHANG,Lingling TONG,Lu GAO,Hongjing CHENG,Minjia SHENG.
Parasitic leiomyoma of abdominal wall complicated with disseminated peritoneal leiomyomatosis : A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2024, 50(5): 1432-1437.
|
| [13] |
Wenqing RUAN,Zerun FU,Yi HUANG,Longyun LI,Yao SUN,Kai LI.
Application of hypotension prediction index in intraoperative hemodynamic management of robot-assisted laparoscopic cystectomy:A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2024, 50(4): 1130-1136.
|
| [14] |
Shaoning KAN,Han WU,Shuangji LI,Jingcheng XIANG,Yuyang LI,Liou JIN,Weiwei LIU.
Simple bone cyst in ipsilateral maxilla and mandible:A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2024, 50(2): 551-555.
|
| [15] |
Qinghua PING,Wenjing ZHU,Jianxin XIA.
Pustular psoriasis treated with secukinumab during pregency: A case report and literature review
[J]. Journal of Jilin University(Medicine Edition), 2023, 49(6): 1599-1603.
|
 )
)